Restricting Carbohydrate Raises Cortisol
Some advocates of low carbohydrate, ketogenic, and "carnivore" diets deny that restricting carbohydrate raises cortisol, triggers the stress response, and suppresses metabolic rate. Here I will review studies providing evidence that limiting or avoiding dietary carbohydrate does in fact raise cortisol levels, trigger the "fight or flight" stress response, and suppress metabolic rate.
Beware that in this article I will use the words "carbohydrate" and "sugar" interchangeably because it is scientifically accurate. All carbohydrate consists of sugars. Starch is simply chains of the simple sugar glucose, and upon digestion it enters your body as the simple sugar, not as starch.
Is Dietary Carbohydrate Essential?
Before diving into evidence that restricting carbohydrate raises cortisol, we need to address this. Proponents of carbohydrate restriction often claim that dietary carbohydrate is not an essential nutrient because the body can produce glucose––sugar––from catabolism of amino acids in the absence of dietary sugar. I feel painfully embarrassed to admit that I was once among them. In The Hypercarnivore Diet (now out of print) I supported that view, citing the following passages from the U.S. National Academies of Science Food and Nutrition Board:
|
“The lower limit of dietary carbohydrate compatible with life apparently is zero, provided that adequate amounts of protein and fat are consumed….There are traditional populations that ingested a high fat, high protein diet containing only a minimal amount of carbohydrate for extended periods of time (Masai), and in some cases for a lifetime after infancy (Alaska and Greenland Natives, Inuits and Pampas indigenous people)…There was no apparent effect on health or longevity…. “The ability of humans to starve for weeks after endogenous glycogen supplies are essentially exhausted is also indicative of the ability of humans to survive without an exogenous supply of glucose or mono saccharides convertible to glucose in the liver (fructose and galactose).”1 |
Thus the line of reasoning:
- Premise 1: Some humans can and do live for lifetimes with very limited carbohydrate intake.
- Premise 2: All humans can starve for weeks without consuming any carbohydrate.
- Conclusion: Therefore, since no human has an absolute requirement for dietary carbohydrate in order to survive, there is no benefit to consuming carbohydrate, and the ideal diet contains little or no carbohydrate.
Again, as a trained philosopher (Master's degree) who used to teach logic at university level, I am embarrassed that I fell for this line of reasoning, but I am grateful that I eventually came to realize the problem with it.
The problem here is that the fact that one can survive for some period of time without something does not prove that one does not need that thing to thrive. There is a very large gap between surviving and thriving.
Although a human can survive without dietary sugars because the liver can produce sugar from dietary protein, that doesn’t prove that you as an individual can thrive without dietary sugars. The fact that we can survive without dietary carbohydrate because we can produce glucose on demand from protein and the glycerol portion of triglycerides is not evidence that dietary sugar is not beneficial or essential.
On the contrary, it is evidence that a constant supply of sugar is vitally important – indeed, critical – to continuation of life. Since an insufficient supply of blood glucose will result in unconsciousness progressing to death, our Creator has designed our metabolism with multiple redundant mechanisms for establishing a floor to glucose levels. At least five hormones– including glucagon, growth hormone, thyroxin, cortisol, and epinephrine (also known as adrenaline)–work together to keep blood sugar from falling too low by stimulating glucogenesis when the dietary supply is short.
Restricting Carbohydrate Raises Cortisol
Although advocates of low carbohydrate and carnivore diets deny, many studies indicate that restricting dietary carbohydrate raises cortisol, activates the stress response, and depresses metabolism.
A study of fasting metabolism in humans found that the adaptive stress response to fasting is a response to restriction of carbohydrate, not calories.2 The study revealed that restricting calories without restricting carbohydrate did not elicit the stress response; and that restricting carbohydrate raises cortisol even without restriction of calories. This means that you can’t prevent the stress response to dietary sugar restriction by simply eating more fat.
Animal studies also show that restricting carbohydrate raises cortisol. Rodents maintained on a low-carbohydrate high-fat ketogenic diet show canonical markers of chronic stress, including increases in basal and stress-stimulated cortisol, increased adrenal sensitivity to adrenocorticotropin hormone, and atrophy of the thymus, which indicates chronic glucocorticoid exposure.3
Studies of children following ketogenic diets to control seizures also show that restricting carbohydrate raises cortisol. In one study, all children consuming a very low carbohydrate ketogenic diet for control of seizures had elevated serum cortisol.4 Authors of this study even postulated that the elevated cortisol level could contribute to the anti-seizure activity of the ketogenic diet.
Studies conducted with otherwise healthy people have shown that even moderately restricting carbohydrate raises cortisol levels. When healthy men consumed a high (44%) protein, moderate (35%) carbohydrate, low (21%) fat diet (based on meat, fish, poultry, and egg whites), their cortisol levels increased and testosterone levels decreased, compared to when they ate a high (70%) carbohydrate, low (20%) fat, moderate (10%) protein diet.5
Increasing dietary protein may also raise cortisol levels. Several studies have shown that high protein meals may increase salivary cortisol levels and may in women reduce sense of well-being.6, 7, 8, , Women may need more dietary sugar than males to obtain well-being. Since both increasing protein and restricting carbohydrate raises cortisol, low carbohydrate high protein diets deliver a one-two punch to trigger the stress response.
Carbohydrate Restriction Activates "Fight or Flight" Stress Response
While restricting carbohydrate raises cortisol levels, it also triggers the fight or flight response. The stress response includes release of catecholamines, including epinephrine and norepinephrine (adrenalin and nor-adrenalin), known as “fight or flight” neurotransmitters. Three prominent low carbohydrate and ketogenic diet advocates have stated that since epinephrine (adrenalin) increases during fasting due to carbohydrate restriction, adrenalin is also “likely to be elevated during nutritional ketosis.”9
These three advocates of carbohydrate restriction went on to cite research indicating that “dietary carbohydrate restriction increases catecholamines at rest and in response to exercise”10, 11, and “the potential for nutritional ketosis to increase catecholamines is further supported by the dependency of the antiseizure effects of ketogenic diets on norepinephrine [noradrenalin].”12
Since ketogenic diets are successfully used as a long-term treatment for seizure disorders, we can conclude that ketogenic diets chronically activate the sympathetic nervous system into the "fight or flight" mode.
In 2019 researchers demonstrated that the acute stress response is mediated by a rise in osteocalcin levels.13 Children on a ketogenic diet for treatment of epilepsy have elevated osteocalcin levels––indicating chronic stress response––and loss of bone mass., Both cortisol and osteocalcin cause loss of bone mass.14, 15
Thus, restricting carbohydrate raises cortisol, osteocalcin, and catecholamines, all part of the stress response.
|
In rodents and humans, sugar consumption reduces the stress response (cortisol level), which is likely why many people crave and preferentially consume sugar or starches when under stress.16 Hence if you crave carbohydrates when eating low carbohydrate diets, this is a signal that the body is under stress. Many people will fight the cravings because they think they indicate an "addiction" to "toxic" sugar. In fact, since sugar is as essential to your life as oxygen, your "addiction" to sugar is on par with your "addiction" to oxygen: you literally can't live without either of them. |
Moreover, sugar is no more toxic than oxygen or water. No one has ever died from acute sugar poisoning. Comparatively, salt is far more toxic than sugar. Dose makes the poison. There are no known toxic effects from consuming 400 or more grams of sugar (carbohydrate) daily, whereas just a 10 grams of salt delivers enough chloride (~6 grams) to have a toxic effect due to formation of hydrochloric acid.
If you restrict your oxygen you will crave fresh air because you actually need oxygen. Similarly your cravings for sugar when you are restricting or avoiding it are strong because you need it. For most people the problem with sugar is that they eat it in refined form, combined with fats (cookies, pastries, candies, etc). Eat less fat and more natural sugar-rich foods: fruits, roots, tubers, whole grains, and legumes.
Restricting Carbohydrate Depresses Metabolism
Some research has suggested that although reducing dietary carbohydrate reduces glycogen stores in the short-term, it has little or no effect on glycogen stores long-term. Advocates of low-carbohydrate diets interpret this as more evidence that no one needs dietary carbohydrate. However, the recovery of glycogen stores on a long-term low carbohydrate diet is evidently a consequence of the diet depressing glucose utilization and metabolic rate and inducing a sense of fatigue in response to low glycogen stores, so that less sugar is used in metabolism and activity and more is saved as glycogen for emergency use.17
The Cost of Restricting Carbohydrate
When I learned that restricting carbohydrate raises cortisol and activates the fight or flight stress response, I understood why I was more irritable, impatient, edgy, and prone to restless sleep and insomnia while I was eating a very low carbohydrate hypercarnivore diet. Restricting carbohydrate raised my cortisol and catecholamine levels, putting me in a more or less constant fight or flight mode. Others may experience more anxiety for the same reason.
When I resumed eating fruits, honey, and some starches and reduced my meat and fat intake, I quickly started sleeping more soundly and had a much happier, calmer and more patient disposition.
Research indicates that you can avoid these adverse effects by ingestion of either a very large amount of protein, or a modest amount of carbohydrate. Evidently, a supply of between 65 and 180 g/day of glucose will prevent the adaptive response that produces these unwanted effects.2 This can come from either an extraordinary amount of surplus dietary protein – such as provided by a total protein intake of 375 g/d – or by a modest direct sugar intake of 65-180 g/d.
Obviously it is more economical and physiological to consume sugar directly than to eat extraordinarily large amounts of animal protein in order to turn it into sugar. An individual engaged in strength training is advised to consume 1.6 g protein per kg of body weight. At about 160 pounds (73 kg), I only need about 117 g of protein daily. To get adequate glucose from animal protein, I would need to consume 258 g of surplus protein daily, which would come from about 36 ounces (1 kg) of meat in addition to the amount that supplies 117 g. That's a little more than 2 pounds of meat.
Assuming I consumed leaner meat, like ground sirloin, because it is higher in protein and lower in fat, I would spend about $10 per day just to get my glucose from meat. The number might seem low to you because I purchase beef by the half directly from a farmer. You would likely spend more, perhaps even $20 per day.
In contrast, I can directly consume 180 g of sugar daily from fruit and inexpensive starches. A pint of orange juice supplies 58 g and costs about $0.50. A pound (454 g) of white potato supplies about 91 g and costs as little as $0.20. Thus, for $0.70 you can obtain 146 g of sugar, plus high vitamin C, folate, potassium and numerous other nutrients not well supplied by even 2 pounds of high quality sirloin.
Thus, a gram of glucose made from animal protein costs about 10 times more than a gram of glucose gotten directly from nutrient-dense plant foods. Why spend $10-20 or more on meat just so your body can turn it into sugar that you can get directly and far more economically––for less than $1.50––from nutrient-dense plants?
Moreover, when you rely on animal protein to obtain glucose, your liver and kidneys bear the burden of dealing with the large amount of nitrogenous waste that results from converting the protein into glucose. This can cause your liver and kidneys to enlarge, a condition that is associated with reduced lifespan.
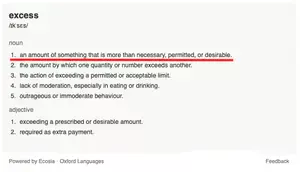
Excess Protein Can Cause Liver and Kidney Hypertrophy
|
In the 1970s, Dr. Ellington Darden, Ph.D., author of Nutrition and Athletic Performance, was a competitive athlete and bodybuilder who won 17 titles including the 1972 Collegiate Mr. America. Up until 1970 he was consuming more than 300 g of protein per day. |
 |
While Darden was studying nutrition and exercise science in the Food and Nutrition Department at Florida State University, one of his professors, Dr. Harold Schendel Ph.D., an expert in protein nutrition, told Darden that was way too much protein and he was wasting his money.
Determined to prove that he needed that protein, Dr. Darden set up a detailed study on his own body. His account of this experiment:
|
"I kept accurate records of my food intake and activity for 60 days, and I even collected my urine during the same period. Afterward, I used the Kjeldahl method for determining nitrogen in my urine, which is a measure of protein utilization. To my surprise, anytime I consumed more than the RDA of protein, the excess was excreted in my urine. Schendel concluded that my kidneys were working overtime to metabolize the excess protein. He also explained that human kidneys and livers show overuse symptoms in the presence of massive amounts of protein. We know from long-term animal studies that high-protein diets will shorten life spans. So I stopped my massive protein diet and immediately felt a surge of energy from unburdening my kidneys and liver. Over the next 2 years, on a carbohydrate-rich diet, I won several of the bodybuilding contests that I’d been trying so hard to win. Adding carbohydrates and subtracting proteins had made a significant difference in my appearance. As a result, I haven’t consumed a high-protein diet since early 1970." Read more from Dr. Darden on protein here. |
|
Clearly, forcing your body to obtain its required glucose from the breakdown of protein puts stress on your liver and kidneys, and takes energy away from other metabolic tasks. No one has provided good evidence that only low carbohydrate high protein diets can produce good health or physical performance. Why sacrifice good attitude, money, bones, liver and kidneys to the false high protein gods? |
 Dr. Darden at his peak. |
Eat Sweets!
In summary:
- Although it is technically true that humans can get all the sugar they need to survive without eating any sugar, this does not mean that it we don't need sugar nor that you will thrive on a diet containing little or no sugar.
- Avoiding sugar forces your body to obtain the sugar it absolutely needs by route of converting protein to sugar. This energetically costly process puts an unnecessary burden on your liver and kidneys, potentially causing them to enlarge and shortening their lifespan.
- Diets low in carbohydrate activate the stress response, including elevation of cortisol, catecholamines (adrenaline and noradrenaline), and osteocalcin. This leads to bone loss and increased susceptibility to anxiety, irritability, impatience, insomnia, agitation, restlessness, and other "fight or flight" responses.
- Meeting your glucose needs by eating surplus protein is highly uneconomical. A gram of sugar derived from animal protein costs about 10 times more than a gram of sugar gotten directly from nutrient-dense plant foods.
- You can relieve and prevent the stress response and increase the overall nutrient density and adequacy of your diet by eating a diet containing plenty of sugar from nutrient-dense, sugar-rich plant foods instead of forcing your body to convert protein into sugar.
|
Confronting all of these facts (among many others) contributed to convincing me that I was foolish to continue eating and promoting a very high protein, high fat, low carbohydrate hypercarnivore diet. I upgraded to eating nutrient-dense sweets, which relieved me of muscle cramping due to potassium deficiency, and has resulted in a great improvement in my psoriasis, my disposition, and my physical performance, among other things. |
NOTES
1. Food and Nutrition Board, National Academy of Sciences. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids. National Academies Press, 2005. Pages 275-6. <https://www.nap.edu/read/10490/chapter/8?term=carbohydrate+requirement#275>
2. Wolfe, R.R.A.K.S. (1992). Carbohydrate restriction regulates the adaptive response to fasting. AJP - Endocrinology and Metabolism, 262, E631
3. Ryan KK, Packard AEB, Larson KR, et al. Dietary Manipulations That Induce Ketosis Activate the HPA Axis in Male Rats and Mice: A Potential Role for Fibroblast Growth Factor-21. Endocrinology. 2018;159(1):400–413. doi:10.1210/en.2017-00486 <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5761593/>
4. Fraser DD, Whiting MB, Andrew RD, et al. Elevated polyunsaturated fatty acids in blood serum obtained from children on the ketogenic diet. Neurology 2003:60:1026-1029.
5. Anderson KE, Rosner W, Khan MS, et al. Diet-hormone interactions: Protein/carbohydrate ratio alters reciprocally the plasma levels of testosterone and cortisol and their respective binding globulins in man. Life Sciences 1987;40(18):1761-1768.
6. Gibson EL, Checkley S, Papadopoulus A, et al. Increased salivary cortisol reliably induced by a protein-rich midday meal. Psychosom Med 1999 Mar-Apr;61(2):214-24. Abstact.
7. Ishizuka B, Quigley ME, Yen SS. Pituitary hormone release in response to food ingestion: evidence for neuroendocrine signals from gut to brain. J Clin Endocrinol Metab 1983 Dec;57(6):1111-6. Abstract.
8. Giovannini C, Sellini M, Manzo G, et al. The influence, in normal subjects, of a high-protein normocaloric diet on the response of cortisol, ACTH, GH, and PRL to insulin hypoglycemia. Boll Soc Ital Biol Sper 1982 Feb;58;58(3-4):121-7. Abstract. Article in Italian.
9. Miller VJ, Villamena FA, Volek JS. Nutritional Ketosis and Mitohormesis: Potential Implications for Mitochondrial Function and Human Health. J Nutr Metab. 2018;2018:5157645. Published 2018 Feb 11. doi:10.1155/2018/5157645 <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5828461/>
10. Langfort J, Pilis W, Zarzeczny R, Nazar K, Kaciuba-Uściłko H. Effect of low-carbohydrate-ketogenic diet on metabolic and hormonal responses to graded exercise in men. J Physiol Pharmacol. 1996 Jun;47(2):361-71. PubMed PMID: 8807563.<https://www.ncbi.nlm.nih.gov/pubmed/8807563> “Both the pre-and post-exercise levels of adrenaline, noradrenaline, and cortisol were enhanced, whilst plasma insulin concentration was decreased on the ketogenic diet."
11. Langfort J, Czarnowski D, Zendzian-Piotrowska M, Zarzeczny R, Górski J. Short-term low-carbohydrate diet dissociates lactate and ammonia thresholds in men. J Strength Cond Res. 2004 May;18(2):260-5. PubMed PMID: 15142017 <https://www.ncbi.nlm.nih.gov/pubmed/15142017>
12. Szot P, Weinshenker D, Rho JM, Storey TW, Schwartzkroin PA. Norepinephrine is required for the anticonvulsant effect of the ketogenic diet. Brain Res Dev Brain Res. 2001 Aug 23;129(2):211-4. PubMed PMID: 11506865.<https://www.ncbi.nlm.nih.gov/pubmed/11506865>
13. Berger JM, Singh P, Khrimian L, et al. Mediation of the Acute Stress Response by the Skeleton. Cell Metabolism 2019 Nov 5;30(5):P890-902, E8. <https://www.cell.com/cell-metabolism/fulltext/S1550-4131(19)30441-3>
14. Sullivan MG. Bone growth affected by ketogenic diet in children with epilepsy. Clinical Neurology News 2013 July 13. <https://www.mdedge.com/clinicalneurologynews/article/76168/pediatrics/bone-growth-affected-ketogenic-diet-children-epilepsy>
15. Simm, P., Bicknell-Royle, J., Lawrie, J., Nation, J., Draffin, K., Stewart, K., Cameron, F., Scheffer, I., & Mackay, M. (2017). The effect of the ketogenic diet on the developing skeleton. Epilepsy Research, 136, 62-66.
16. Laugero, K. (2001). A New Perspective on Glucocorticoid Feedback: Relation to Stress, Carbohydrate Feeding and Feeling Better. Journal of Neuroendocrinology 2001:13(9):827-35.
17. Winwood-Smith HS, Franklin CE, White CR. Low-carbohydrate diet induces metabolic depression: a possible mechanism to conserve glycogen. Am J Physiol Regul Integr Comp Physiol 2017;313:R347–R356. doi:10.1152/ajp-regu.00067.2017.
Recent Articles
-
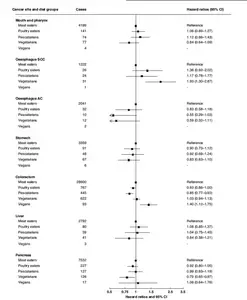
Vegans Have The Highest Colorectal Cancer Risk? No
Mar 13, 26 05:37 PM
Do vegans have the highest colorectal cancer risk as recent Dunneram study claims? No! -
Ancient Roman Soldier Diet
Apr 14, 25 05:19 PM
A discussion of the ancient Roman soldier diet, its staple foods and nutritional value, and a vegan minimalist version. -
High Protein Chocolate Tofu Pudding
Jul 01, 24 12:41 PM
A delicious high protein chocolate tofu pudding. -
Vegan Macrobiotic Diet For Psoriasis
Sep 05, 23 06:36 PM
Vegan macrobiotic diet for psoriasis. My progress healing psoriasis with a vegan macrobiotic diet. -
How Every Disease Develops
Aug 04, 23 06:22 PM
How every disease develops over time, according to macrobiotic medicine. -
Why Do People Quit Being Vegan?
Jun 28, 23 08:04 PM
Why do people quit being vegan? How peer pressure and ego conspire against vegans. -
Powered By Plants
Mar 16, 23 08:01 PM
Powered By Plants is a book in which I have presented a lot of scientific evidence that humans are designed by Nature for a whole foods plant-based diet. -
Carnism Versus Libertarianism
Dec 30, 22 01:55 PM
Carnism Versus Libertarianism is an e-book demonstrating that carnism is in principle incompatible with libertarianism, voluntaryism, and anarchism.