Do Vegans Have The Highest Colorectal Cancer Risk?
Do vegans have the highest colorectal cancer risk, and the highest risks for several other cancers, as alleged by 2026 study by Dunneram and colleagues?
Not likely. Dunneram and colleagues probably produced a false positive association between vegan diets and increased cancer risks by over-adjustments to their data.
In 2026 Dunneram and colleagues published a study of vegetarian diets and cancer risk, based on analysis of 1.8 million people in nine prospective studies on three continents.1 They reported that, compared to meat-eaters, vegans had lower relative risks of cancers of mouth and pharynx, esophagus AC, stomach, liver, breast, prostate, kidney, and bladder, and similar risks for pancreas, endometrium, ovary, and multiple myeloma.
However, Dunneram and colleagues alleged that the vegans studied had a 93% greater relative risk of squamous cell carcinoma of the esophagus, a 40% greater relative risk of colorectal cancer, a 23% greater relative risk of non-Hodgkin lymphoma, and a 48% greater relative risk of leukemia. Here are their tables in which they suggest that vegans have highest colorectal cancer risk:
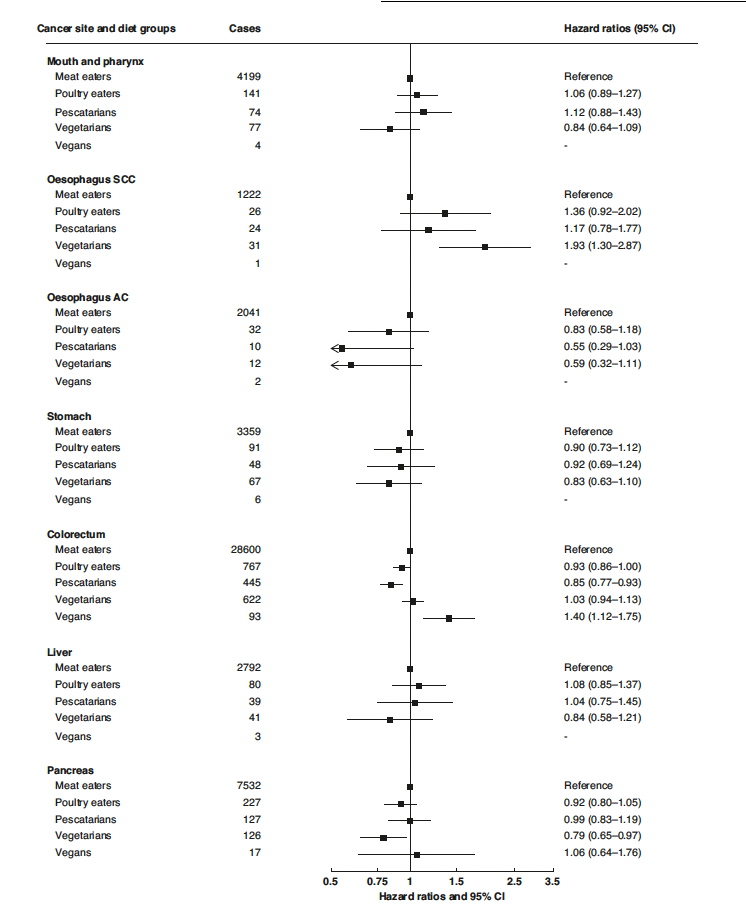
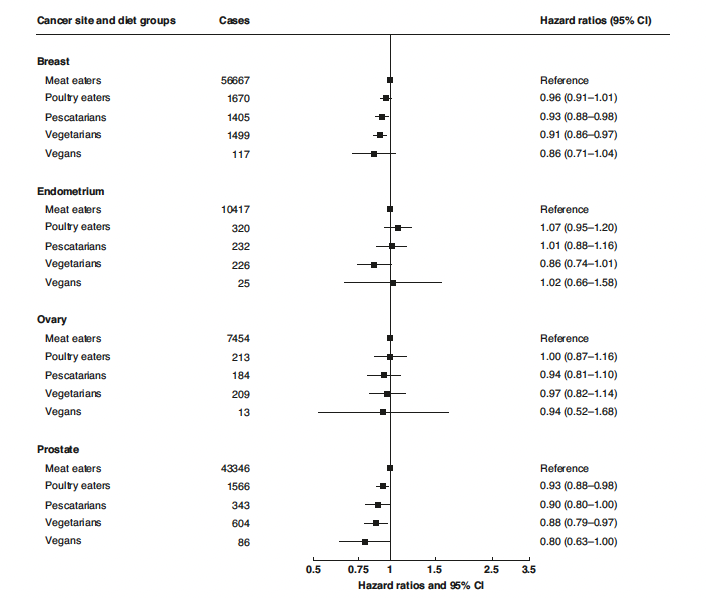
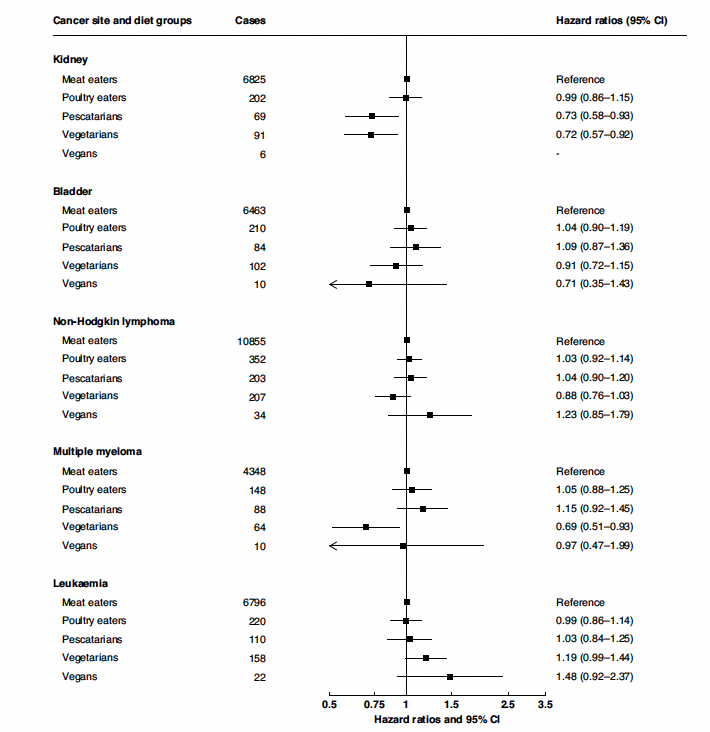
These tables list the number of cases of each type of cancer in each diet group. Dunneram and colleagues reported the total number of subjects in each diet group:
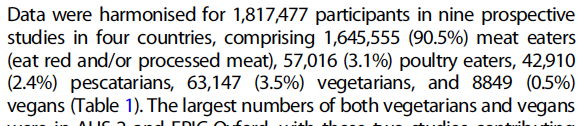
Using this data we can calculate the absolute risks for each of the cancers for which they claimed vegans had much elevated relative risks. For clarity, the absolute risk is the number of cases per 100 or 1000; whereas relative risk compares absolute risks between groups. I calculated the absolute risks as shown in the following table:
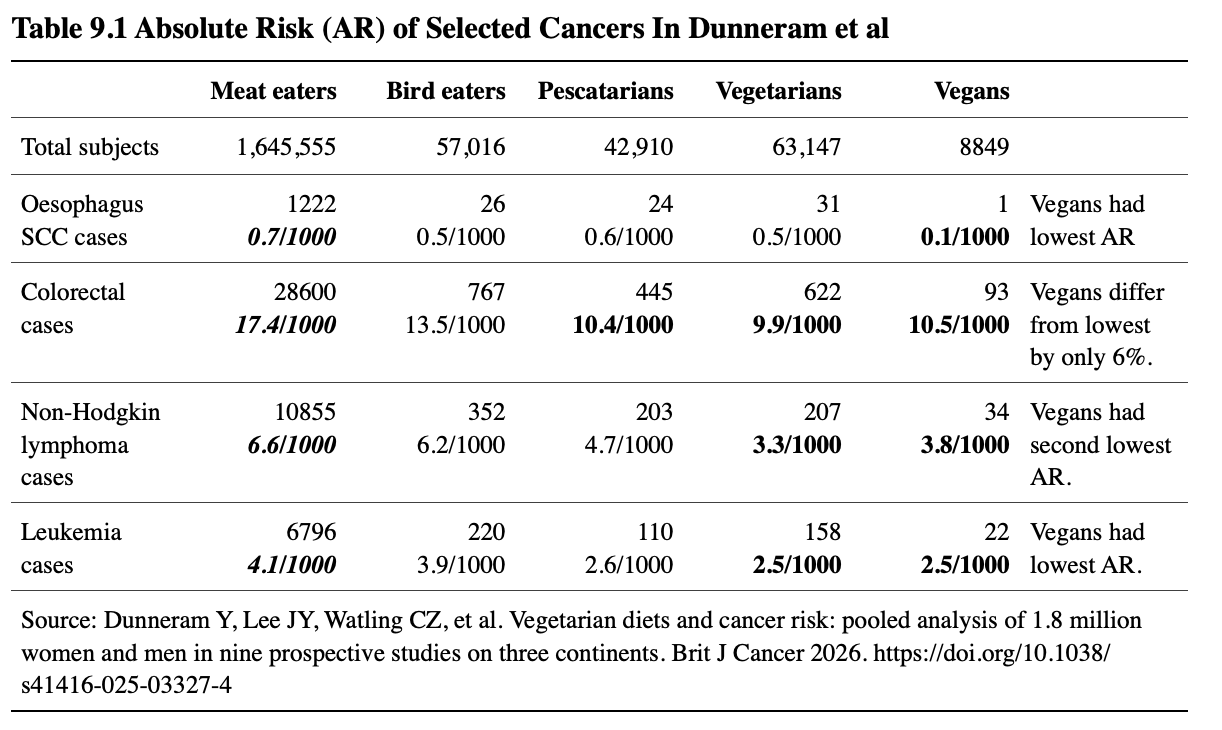
As shown, in fact the meat-eaters had the highest absolute risks for all of these cancers, while vegans had the lowest absolute risk of squamous cell carcinoma of the esophagus and leukemia, the second lowest absolute risk of non-Hodgkin lymphoma, and vegans, vegetarians, and pescatarians all had similar absolute risks for colorectal cancer, all lower than meat-eaters. To the point, compared to vegans, meat-eaters’ absolute risks for these cancers were: 7 times higher for esophageal SCC, ~70% higher for colorectal, 74% higher for non-Hodgkin lymphoma, and 64% higher for leukemia.
So, how did they get their conclusions that vegans, not meat-eaters, had the highest relative risks for these cancers?
What Created The Illusion That Vegans Have The Highest Colorectal Cancer Risk?
Dunneram and colleagues probably produced the illusion that vegans have the highest colorectal cancer risk, as well as the highest risks for several other cancers, by over-adjustment of their data.
Specifically, they adjusted the data for body mass index and history of type 2 diabetes. Both body mass index and type 2 diabetes are both positively associated with increased risk of developing colorectal cancer [2, 3, 4], while flesh-free diets are strongly associated with low body mass index and diabetes [5].
In addition, in the case of esophageal SCC, there was only 1 case in the vegan group. Dunneram and colleagues claimed that vegans have a nearly doubled relative risk for this cancer compared to meat eaters, whereas in fact the meat-eaters had a 7 times greater absolute risk for this cancer compared to vegans. Obesity and diabetes dramatically increase the risk of esophageal carcinoma [6, 7].
Obesity also increases the risk of leukemia and probably increases the risk of non-Hodgkin's lymphoma [8, 9].
Therefore, it is very likely that, by adjusting for body mass index and diabetes risk, Dunneram and colleagues deceptively erased the true negative association and manufactured a false positive association between flesh-free diets and several cancers including colorectal. If so, this is an example of over-adjustment bias [10].
Since the data provided by Dunneram and colleagues indicates that vegan diets very likely reduce the absolute risk of these cancers, by removing the influence of BMI and diabetes on the outcome by data adjustment, one can create the illusion that a flesh-free diet not only does not protect against these cancers, but increases the risk, but this is likely a statistical artifact.
Dunneram and colleagues spill a lot of ink trying to convince the reader that vegans may have increased risk of these cancers due to nutrient deficiencies. However, their claim that vegans have increased relative risk of these cancers is itself dubious, probably based on over-adjustment bias, and at variance with expectations based on the large bodies of previous research on these cancers, their links to obesity or diabetes, and the well established links between consumption of animal flesh and obesity and diabetes.
In summary, this study did not provide good evidence that vegans have the highest colorectal cancer risk. It is more likely that it merely demonstrated that study authors can manufacture false positive associations and erase true negative associations by over-adjusting data.
Notes
1. Dunneram Y, Lee JY, Watling CZ, et al. Vegetarian diets and cancer risk: pooled analysis of 1.8 million women and men in nine prospective studies on three continents. Brit J Cancer 2026.
https://www.nature.com/articles/s41416-025-03327-4#Sec16
2. Mandic M, Li H, Safizadeh F, et al. Is the association of overweight and obesity with colorectal cancer underestimated? An umbrella review of systematic reviews and meta-analyses. Eur J Epidemiol. 2023 Feb;38(2):135-144. doi: 10.1007/s10654-022-00954-6. Epub 2023 Jan 21. Erratum in: Eur J Epidemiol. 2024 Feb;39(2):231. doi: 10.1007/s10654-023-01092-3. PMID: 36680645; PMCID: PMC9905196.
3. Lawler T, Walts ZL, Steinwandel M, et al Type 2 Diabetes and Colorectal Cancer Risk. JAMA Netw Open. 2023 Nov 1;6(11):e2343333. doi: 10.1001/jamanetworkopen.2023.43333. PMID: 37962884; PMCID: PMC10646729.
4. Li Z, Chen H, Fritz CDL, et al. Type 2 Diabetes and Risk of Early-Onset Colorectal Cancer. Gastro Hep Adv. 2022 Feb 3;1(2):186-193. doi: 10.1016/j.gastha.2021.10.009. PMID: 39131121; PMCID: PMC11308819.
5. Baroni L, Rizzo G, Galchenko AV, Zavoli M, Serventi L, Battino M. Health Benefits of Vegetarian Diets: An Insight into the Main Topics. Foods. 2024 Jul 29;13(15):2398. doi: 10.3390/foods13152398. PMID: 39123589; PMCID: PMC11311397.
6. Chen Q, Zhuang H, Liu Y. The association between obesity factor and esophageal caner. J Gastrointest Oncol. 2012 Sep;3(3):226-31. doi: 10.3978/j.issn.2078-6891.2012.026. PMID: 22943013; PMCID: PMC3418533.
7. Xu B, Zhou X, Li X, Liu C, Yang C. Diabetes mellitus carries a risk of esophageal cancer: A meta-analysis. Medicine (Baltimore). 2017 Sep;96(35):e7944. doi: 10.1097/MD.0000000000007944. PMID: 28858123; PMCID: PMC5585517.
8. Tsilingiris D, Vallianou NG, Spyrou N, Kounatidis D, Christodoulatos GS, Karampela I, Dalamaga M. Obesity and Leukemia: Biological Mechanisms, Perspectives, and Challenges. Curr Obes Rep. 2024 Mar;13(1):1-34. doi: 10.1007/s13679-023-00542-z. Epub 2023 Dec 30. PMID: 38159164; PMCID: PMC10933194.
9. Skibola CF. Obesity, diet and risk of non-Hodgkin lymphoma. Cancer Epidemiol Biomarkers Prev. 2007 Mar;16(3):392-5. doi: 10.1158/1055-9965.EPI-06-1081. Epub 2007 Mar 2. PMID: 17337642; PMCID: PMC2819159.
10. Schisterman EF, Cole SR, Platt RW. Overadjustment bias and unnecessary adjustment in epidemiologic studies. Epidemiology. 2009 Jul;20(4):488-95. doi: 10.1097/EDE.0b013e3181a819a1. PMID: 19525685; PMCID: PMC2744485.
Recent Articles
-
Vegans Have The Highest Colorectal Cancer Risk? No
Mar 13, 26 05:37 PM
Do vegans have the highest colorectal cancer risk as recent Dunneram study claims? No! -
Ancient Roman Soldier Diet
Apr 14, 25 05:19 PM
A discussion of the ancient Roman soldier diet, its staple foods and nutritional value, and a vegan minimalist version. -
High Protein Chocolate Tofu Pudding
Jul 01, 24 12:41 PM
A delicious high protein chocolate tofu pudding. -
Vegan Macrobiotic Diet For Psoriasis
Sep 05, 23 06:36 PM
Vegan macrobiotic diet for psoriasis. My progress healing psoriasis with a vegan macrobiotic diet. -
How Every Disease Develops
Aug 04, 23 06:22 PM
How every disease develops over time, according to macrobiotic medicine. -
Why Do People Quit Being Vegan?
Jun 28, 23 08:04 PM
Why do people quit being vegan? How peer pressure and ego conspire against vegans. -
Powered By Plants
Mar 16, 23 08:01 PM
Powered By Plants is a book in which I have presented a lot of scientific evidence that humans are designed by Nature for a whole foods plant-based diet. -
Carnism Versus Libertarianism
Dec 30, 22 01:55 PM
Carnism Versus Libertarianism is an e-book demonstrating that carnism is in principle incompatible with libertarianism, voluntaryism, and anarchism.